 Gestational diabetes is a type of diabetes which some women may develop during pregnancy. Almost 2-7% of all expecting mothers will develop gestational diabetes and this makes it one of the most common pregnancy complications
In a nut shell, gestational diabetes occurs when your digestive system breaks down most of your food into a type of sugar called glucose. The glucose enters your bloodstream and then insulin, which is a hormone produced by your pancreas, provides fuel for the cells of your body. Gestational diabetes causes the glucose to stay in your blood instead of moving into your cells and getting converted to energy.
The hormones which are produced while you are pregnant make it harder for your body to use insulin, so your pancreas produces more of it. Now, for most pregnant women, this isn’t a problem, as your need for insulin increases, your pancreas dutifully secretes more of it. Gestational diabetes occurs when your pancreas simply cannot produce enough insulin, which results in a increase in the blood glucose levels getting too high.
Gestational diabetes is a type of diabetes which some women may develop during pregnancy. Almost 2-7% of all expecting mothers will develop gestational diabetes and this makes it one of the most common pregnancy complications
In a nut shell, gestational diabetes occurs when your digestive system breaks down most of your food into a type of sugar called glucose. The glucose enters your bloodstream and then insulin, which is a hormone produced by your pancreas, provides fuel for the cells of your body. Gestational diabetes causes the glucose to stay in your blood instead of moving into your cells and getting converted to energy.
The hormones which are produced while you are pregnant make it harder for your body to use insulin, so your pancreas produces more of it. Now, for most pregnant women, this isn’t a problem, as your need for insulin increases, your pancreas dutifully secretes more of it. Gestational diabetes occurs when your pancreas simply cannot produce enough insulin, which results in a increase in the blood glucose levels getting too high.
Is having Gestational Diabetes going to affect my pregnancy?
With modern technology and medicine standards, most women who develop diabetes during pregnancy go on to have healthy babies. Your healthcare provider will monitor you closely and you’ll most likely be able to keep your blood sugar levels under control with diet and exercise, and by getting insulin shots if you need them. However, if your diabetes is not monitored closely, and it is not kept under control, then the results for both you and your baby can become very complicated.Will my baby be monitored during my pregnancy to avoid complications?
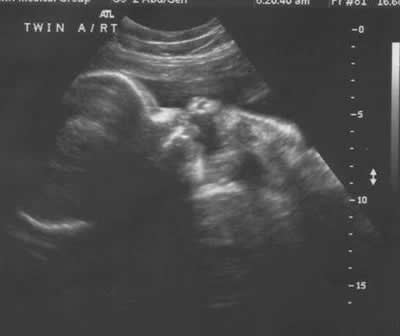
Your healthcare provider will ensure that your baby is monitored more intensively, especially during the remaining 2-3 months of your pregnancy. You may be asked to count your baby’s kicks and your healthcare provider will also tell you just when exactly you should call him/her for any signs that your baby in not as active as he or she should be. Lets say that you are simply not able to control your glucose level and it remains high enough that you need to be given, or to take insulin, or perhaps suffer any other complications as a result, then your healthcare provider will surely have your baby’s heart monitored or periodic ultrasounds done to ensure that your baby is in good health.How will I know if I have Gestational Diabetes?
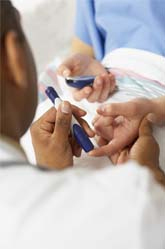
You may notice that you’re more thirsty, hungry or tired than usual or that you have to urinate more frequently, however, these are also some of the common pregnancy signs during a normal pregnancy as well. It is for this very simply reason that most pregnant women will be given a glucose screening test for it between 24 and 28 weeks. If, however you are deemed to be at risk of having gestational diabetes, then your care giver should recommend that you have a glucose at your first prenatal visit, as well as the 24-28 week tests. Should the screening test indicate the possibility of gestational diabetes, then you will be required to take a glucose tolerance test.Am I at risk of having Gestational Diabetes?
According to the American Diabetes Association, you’re considered at high risk for this condition (and should be screened early) if:- You’re obese (your body mass index is over 30).
- You have a history of gestational diabetes (you’ve had the condition in a previous pregnancy).
- You have a strong family history of diabetes.
- You’re found to have sugar in your urine (your urine is tested at each prenatal visit).
- You’ve previously given birth to a big baby (some use 8 pounds, 13 ounces as the cut off; others use 9 pounds, 14 ounces).
- You’ve had an unexplained stillbirth.
- You’ve had a baby with a birth defect.
- You have high blood pressure (hypertension).
How is Gestational Diabetes managed?
It depends on how serious your condition is. You’ll need to keep diligent track of your glucose levels, using a home glucose meter or strips. There are a number of other ways of controlling your diabetes, and these include:- Eating a well-planned diet can help you keep those levels where they should be
- Follow an approved exercise routine
- Recently, some practitioners have been prescribing oral medications (such as glyburide or metformin) instead of insulin for gestational diabetes, but the safety and effectiveness of these drugs is still a matter of debate.
Gestational Diabetes